What does HPV diagnosis mean STI? Understanding the connection between Human Papillomavirus (HPV) and sexually transmitted infections (STIs) is crucial for your health. This comprehensive guide explores HPV diagnosis, its relationship with STIs, potential implications, and preventive strategies.
HPV, a common viral infection, can sometimes lead to various health concerns. This guide dives deep into the different types of HPV, the diagnostic methods, and the potential co-infections with other STIs. We’ll cover symptoms, testing, and treatment options, ultimately empowering you with the knowledge you need.
Understanding HPV Diagnosis
Human Papillomavirus (HPV) is a common sexually transmitted infection (STI) affecting both men and women. It’s crucial to understand the various aspects of HPV diagnosis to ensure appropriate management and treatment. A correct diagnosis allows for proactive steps to prevent potential health complications.
Human Papillomavirus (HPV) Overview
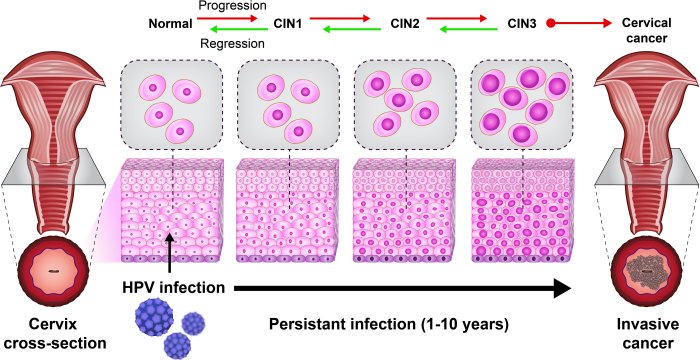
Human Papillomavirus (HPV) encompasses a large family of viruses. Some types of HPV cause genital warts, while others can increase the risk of developing certain cancers, such as cervical, anal, or oropharyngeal cancers. Understanding the different types of HPV and their potential implications is essential for preventative measures and early detection.
HPV Types and Health Implications
Numerous HPV types exist, categorized as either low-risk or high-risk. Low-risk types primarily cause genital warts, which are typically benign but can be unsightly and uncomfortable. High-risk types, on the other hand, are linked to a higher risk of developing cancerous cells in the cervix, anus, penis, or throat. Examples include HPV types 16 and 18, which are strongly associated with cervical cancer.
It’s important to remember that not all HPV infections progress to cancer. Many infections resolve on their own, often without any noticeable symptoms.
Methods of Diagnosing HPV Infections
Several methods are used to diagnose HPV infections. These range from visual inspections to laboratory-based tests. Visual examinations can identify visible genital warts. Molecular tests detect the presence of HPV DNA in samples, while serological tests measure antibodies against HPV in the blood.
Common Symptoms Associated with HPV Infections
Symptoms of HPV infections can vary widely. Some individuals experience no symptoms at all, while others may develop genital warts, which can appear as small, fleshy bumps or clusters of bumps in the genital area. In some cases, there may be a precancerous lesion, which is often asymptomatic. Early detection is critical in preventing progression to cancer.
Comparison of Diagnostic Tests for HPV
Different diagnostic tests for HPV have varying strengths and weaknesses. Some tests are more effective at detecting specific HPV types, while others are better at identifying the presence of precancerous lesions. Choosing the right test depends on the individual’s specific situation and the goals of the diagnosis.
Diagnostic Methods Comparison Table
| Test | Strengths | Weaknesses | Accuracy |
|---|---|---|---|
| Visual Inspection (for genital warts) | Simple, quick, and inexpensive. Can identify visible lesions. | Only detects visible warts. Doesn’t identify all HPV types or precancerous changes. Subjectivity in interpretation may occur. | Moderate |
| Molecular Tests (HPV DNA detection) | Highly sensitive in detecting the presence of HPV DNA. Can identify specific HPV types. | Can be expensive and may require specialized laboratory equipment. Doesn’t always indicate active infection. | High |
| Serological Tests (Antibody Detection) | Can indicate prior exposure to HPV. | Less sensitive than DNA tests for identifying current infection. Not widely used for routine HPV diagnosis. | Moderate |
HPV Diagnosis and STIs: What Does Hpv Diagnosis Mean Sti
HPV, or human papillomavirus, is a common sexually transmitted infection (STI) that can have various impacts on health. Understanding its connection to other STIs is crucial for effective prevention and management. While HPV itself often doesn’t cause noticeable symptoms, its presence can increase the risk of acquiring or experiencing other sexually transmitted infections.The relationship between HPV and other STIs isn’t one of direct causation but rather one of shared risk factors and potential co-infection.
Individuals who are infected with HPV often have a weakened immune response in the genital area, making them more susceptible to other STIs. This shared vulnerability underscores the importance of comprehensive STI testing and preventative measures.
Connection Between HPV and Other STIs
HPV infection can create a favorable environment for other STIs to proliferate. The inflammation and damage caused by some HPV types can disrupt the natural defenses of the genital tract, increasing susceptibility to bacterial or viral infections. This vulnerability highlights the significance of comprehensive STI testing to identify and address any potential co-infections.
Overlap and Co-infections
Co-infection, where an individual has simultaneous infections with multiple STIs, is a significant concern. A common scenario is the presence of HPV alongside chlamydia or gonorrhea. These infections can exacerbate each other’s symptoms and complicate treatment. For example, genital warts caused by HPV can become more irritated or inflamed if a person also has a bacterial STI.
Importance of Comprehensive STI Testing
Regular STI testing is crucial for identifying and managing both HPV and other STIs effectively. It’s not enough to just test for HPV; testing for other common STIs, like chlamydia, gonorrhea, and syphilis, is equally important. This comprehensive approach ensures early detection and appropriate treatment, preventing potential complications and the spread of infections.
Comparison of Symptoms and Testing Methods
| Condition | Symptoms | Testing Methods |
|---|---|---|
| HPV | Genital warts (visible bumps or growths), sometimes no noticeable symptoms, in some cases cervical abnormalities (detected through Pap smears). | Pap smear (for cervical abnormalities), visual inspection for warts, molecular tests (detecting HPV DNA). |
| Chlamydia | Often asymptomatic, sometimes includes vaginal discharge, pain during urination, pain during sex, or lower abdominal pain. | Urine test, swab of the infected area. |
Implications of HPV Diagnosis
An HPV diagnosis, while not always immediately alarming, necessitates careful consideration of its implications for individual health. Understanding these implications is crucial for proactive management and ensuring optimal well-being. It’s important to remember that many HPV infections are transient and resolve without causing any significant health problems. However, persistent infections can lead to serious complications, highlighting the importance of ongoing monitoring and appropriate medical intervention.The implications of an HPV diagnosis extend beyond the immediate discomfort or inconvenience.
It’s a reminder that sexual health is an important aspect of overall health, and prompt and informed action is key to managing potential risks effectively. The long-term consequences can vary depending on the specific HPV type, the individual’s immune response, and lifestyle factors.
Significance for Individual Health
An HPV diagnosis signals the presence of a sexually transmitted infection (STI) caused by the human papillomavirus. While many HPV infections are asymptomatic and clear up on their own, some can persist and lead to potentially serious health complications. The significance lies in recognizing the potential for progression to more severe conditions, such as cervical cancer (in women) or other anogenital cancers (in both men and women).
Early detection and appropriate management are essential to minimize these risks.
Potential Long-Term Health Consequences
Persistent HPV infections, particularly those caused by high-risk types, can increase the risk of developing various cancers. These cancers include cervical cancer, vaginal cancer, vulvar cancer, penile cancer, anal cancer, and oropharyngeal cancer. The risk varies depending on the specific HPV type and individual factors. For example, women with persistent HPV infections are at a significantly increased risk of developing cervical cancer.
An HPV diagnosis, meaning Human Papillomavirus, isn’t automatically an STI (sexually transmitted infection) diagnosis. While some HPV types can lead to STIs, a proper diagnosis requires further testing to identify the specific strain and determine its potential health implications. This is crucial in understanding the implications and treatment options. Recent news about Pam Bondi’s attorney general hearing regarding Trump, pam bondi attorney general hearing trump , highlights the complexities of legal and public health issues.
Regardless, getting tested and understanding your HPV status is essential for informed decisions about your health.
Importance of Follow-up Care and Monitoring
Regular follow-up care and monitoring are critical after an HPV diagnosis. This involves regular check-ups with a healthcare provider, potentially including Pap smears (for women), visual examinations, and other relevant tests as advised. The frequency and type of follow-up care will depend on the specific HPV type, the individual’s risk factors, and the results of initial tests.
Available Treatment Options
Treatment options for HPV vary depending on the presence of symptoms and the severity of the infection. In most cases, HPV infections resolve on their own without specific treatment. However, in cases where the infection persists, or if there are associated symptoms or complications, treatment options may include topical medications, surgical interventions, or other targeted therapies. The choice of treatment will be determined by a healthcare provider after a comprehensive evaluation.
An HPV diagnosis, meaning Human Papillomavirus, can sometimes be concerning, especially when it comes to sexually transmitted infections (STIs). Understanding the complexities of HPV is crucial, but so too is knowing the fascinating history of North Carolina as a swing state, north carolina swing state history. While the political landscape of a state doesn’t directly impact a medical diagnosis, it’s interesting to see how different factors influence public health awareness and how these issues affect us all.
Ultimately, an HPV diagnosis requires careful consideration of individual circumstances and professional medical guidance.
Typical Management Process After an HPV Diagnosis
| Stage | Action | Description |
|---|---|---|
| Initial Diagnosis | Diagnosis confirmation, risk assessment | Confirm HPV type, evaluate risk factors (age, sexual history, etc.). |
| Follow-up Appointments | Regular check-ups, screenings | Pap smears (for women), colposcopy, or other appropriate examinations to monitor the infection and detect any potential complications. |
| Treatment (if necessary) | Topical medications, surgery, or other therapies | If the infection persists or complications arise, targeted therapies will be considered. |
| Ongoing Monitoring | Regular check-ups, screenings, lifestyle changes | Continued monitoring to ensure the infection is under control and to detect any potential complications early. Lifestyle changes (e.g., quitting smoking) might be recommended. |
Prevention and Management Strategies
Navigating an HPV diagnosis can be overwhelming, but proactive steps can significantly reduce the risk of complications and improve overall well-being. This section delves into preventative measures, emphasizing vaccination and lifestyle choices, and comparing different strategies for managing HPV.Understanding the multifaceted approach to HPV management is crucial. Effective prevention and management strategies are essential for mitigating the risks associated with HPV infection and promoting long-term health.
Preventative Measures to Reduce HPV Risk
Various strategies are available to reduce the risk of HPV infection. These range from vaccination to lifestyle modifications and include preventive measures like safe sexual practices and regular screenings. Prioritizing these measures can contribute significantly to lowering the risk of HPV-related complications.
The Importance of Vaccination
HPV vaccination is a cornerstone of preventative care. It significantly reduces the risk of developing HPV infections and associated health problems. Vaccination is highly effective in preventing infection with several high-risk HPV types linked to cancer development.
Comparison of Preventative Strategies
Different preventative strategies offer varying levels of protection. Safe sexual practices, such as using condoms consistently and correctly, are crucial in reducing the risk of transmission. Furthermore, regular screening, while not a direct preventative measure, is critical in early detection and treatment of potential complications. Vaccination, however, offers the most targeted protection against specific HPV types.
Role of Lifestyle Factors in Managing HPV
Maintaining a healthy lifestyle can positively influence the body’s ability to manage HPV. A balanced diet rich in fruits and vegetables, regular exercise, and stress management techniques can contribute to a stronger immune system, potentially aiding in the body’s natural defense against HPV. This is in addition to avoiding smoking and excessive alcohol consumption, both known to compromise immune function.
Recommended Preventative Measures and Their Effectiveness
| Prevention Method | Effectiveness | Considerations |
|---|---|---|
| Vaccination | Highly effective in preventing infection with targeted HPV types. Studies have shown a significant reduction in HPV-related diseases among vaccinated individuals. | Vaccination is most effective when administered before exposure to HPV. Boosters may be required for optimal protection. |
| Safe Sexual Practices | Reduces the risk of HPV transmission. Consistent and correct condom use can significantly lower the chances of infection. | Condoms do not provide 100% protection against HPV transmission. Other factors like the presence of genital warts can also affect the spread. |
| Regular Screening | Important for early detection of precancerous lesions and cancers linked to HPV. | Screening is recommended for individuals at higher risk, but it does not prevent infection. |
| Healthy Lifestyle | A healthy diet, regular exercise, and stress management contribute to a stronger immune system, potentially aiding in the body’s natural response to HPV. | Lifestyle changes are not a guaranteed prevention method, but they contribute to overall health and well-being. |
Addressing Common Concerns
Navigating an HPV diagnosis can be emotionally challenging. Understanding the common anxieties, misconceptions, and the support available is crucial for a positive and informed approach to managing this health concern. This section will address these concerns, empowering you with the knowledge and resources to move forward.Many individuals experience a range of emotions, including fear, anxiety, and uncertainty following an HPV diagnosis.
This is a normal response, and it’s essential to acknowledge and address these feelings. Open communication, education, and support networks play vital roles in managing these emotions effectively.
Common Questions and Misconceptions
HPV is a common sexually transmitted infection, and while it often resolves on its own, it can sometimes lead to serious health issues. Understanding the facts can help dispel misinformation and reduce anxiety. Many people associate HPV with severe health consequences. However, most HPV infections are asymptomatic and resolve without intervention.
An HPV diagnosis, meaning you have a sexually transmitted infection (STI), can be concerning, but it’s important to remember that many STIs are treatable. Recent news about the rfk confirmation hearing vaccines highlights the ongoing discussion surrounding public health and preventative measures, which is relevant to understanding how to manage and treat STIs like HPV. Ultimately, a proper diagnosis and treatment plan from a healthcare professional is key to managing any STI.
Psychological Impact of an HPV Diagnosis
The emotional impact of an HPV diagnosis can vary significantly. Individuals may experience feelings of guilt, shame, or fear, particularly if they feel the diagnosis reflects poorly on their character. It’s important to remember that HPV is a common infection and does not define a person’s worth or character. Seeking support from trusted individuals or professionals is crucial for navigating these emotions.
Resources for Support and Guidance
A wide range of resources are available to provide support and guidance during this time. These resources may include support groups, online forums, or counseling services. Reaching out to healthcare providers, family members, and trusted friends can also be beneficial. Remember, you are not alone in this experience.
Importance of Open Communication with Healthcare Providers
Open and honest communication with healthcare providers is essential for managing an HPV diagnosis effectively. Discuss concerns, ask questions, and seek clarification on treatment options and long-term management strategies. This collaborative approach ensures that you receive the best possible care and support. Be prepared to ask questions about the diagnosis, its implications, and potential treatment options.
Finding Reliable Information Sources
Navigating the vast amount of information available online requires discernment. Look for reputable sources such as the Centers for Disease Control and Prevention (CDC), the World Health Organization (WHO), and other medical organizations. These resources provide evidence-based information and guidance on managing HPV. Avoid unreliable websites or social media posts as they may spread misinformation.
Illustrative Case Studies
Understanding HPV diagnosis requires looking at real-world examples. This section presents a fictional case study to illustrate the diagnostic process, timeline, and factors influencing management. It also highlights the critical role of accurate diagnosis in effective patient care.The following case study focuses on a 25-year-old female presenting with abnormal cervical cytology results. This is a common scenario in HPV diagnosis, and the steps taken in this case are representative of typical clinical practice.
Case Study: Sarah’s Journey, What does hpv diagnosis mean sti
Sarah, a 25-year-old woman, presented to her gynecologist with a routine Pap smear. The results revealed abnormal cervical cells, specifically atypical squamous cells of undetermined significance (ASCUS). This prompted further investigation to determine the cause.
Diagnostic Process
The initial abnormal Pap smear result triggered a series of diagnostic steps. A colposcopy, a procedure that uses a magnifying instrument to examine the cervix, was performed. The colposcopy revealed an area of abnormal tissue that was biopsied. This tissue sample was then sent to a laboratory for analysis. The laboratory performed a DNA test for HPV to identify the presence and type of HPV infection.
Timeline for Diagnosis and Treatment
The timeline for Sarah’s diagnosis varied depending on the availability of testing and the physician’s schedule. Typically, the entire process from the initial Pap smear to a definitive diagnosis and treatment plan can take several weeks, or even months, depending on the complexity of the case.
- Initial Pap smear: Week 1
- Colposcopy and biopsy: Week 2
- Laboratory analysis and HPV DNA testing: Week 3-4
- Diagnosis confirmation and treatment plan: Week 5-6
Factors Influencing Management Approach
Several factors influenced the management approach for Sarah’s case. These included the specific type of HPV detected, the severity of the cervical abnormality, and Sarah’s overall health status. For instance, if a high-risk HPV type was identified, a more aggressive treatment approach might be necessary. The physician’s experience and the local healthcare guidelines also play a role.
- HPV Type: High-risk HPV types are associated with a higher risk of developing cervical cancer and may necessitate more intensive treatment protocols. Low-risk types might require less aggressive intervention.
- Severity of abnormality: The severity of the abnormal cells identified in the Pap smear or colposcopy dictates the level of concern and urgency of treatment.
- Patient’s overall health: Co-existing medical conditions could affect the treatment options and the timing of interventions.
Importance of Accurate Diagnosis
Accurate diagnosis is crucial in clinical practice for several reasons. It ensures appropriate treatment, avoids unnecessary interventions, and reduces the risk of complications. It also facilitates effective patient counseling and reduces the likelihood of progression to more severe conditions. Inaccurate diagnosis can lead to delayed or inappropriate treatment, potentially impacting patient outcomes.
Illustrative Image: Cervical HPV Lesion
Imagine a magnified view of the cervix. A small, slightly raised, and irregular area of tissue is visible. The color of the lesion may vary, ranging from slightly pinkish to white. This is an example of an HPV lesion, which can be further examined and analyzed to determine the type and severity.
Accurate diagnosis of HPV infection is critical for timely and effective management.
Last Word
In conclusion, understanding HPV diagnosis, particularly in the context of STIs, is essential for proactive health management. Early detection, informed choices, and open communication with healthcare providers are key. By arming yourself with knowledge, you can make well-informed decisions about your health and well-being. Remember, accurate information and support are vital in navigating this topic.
